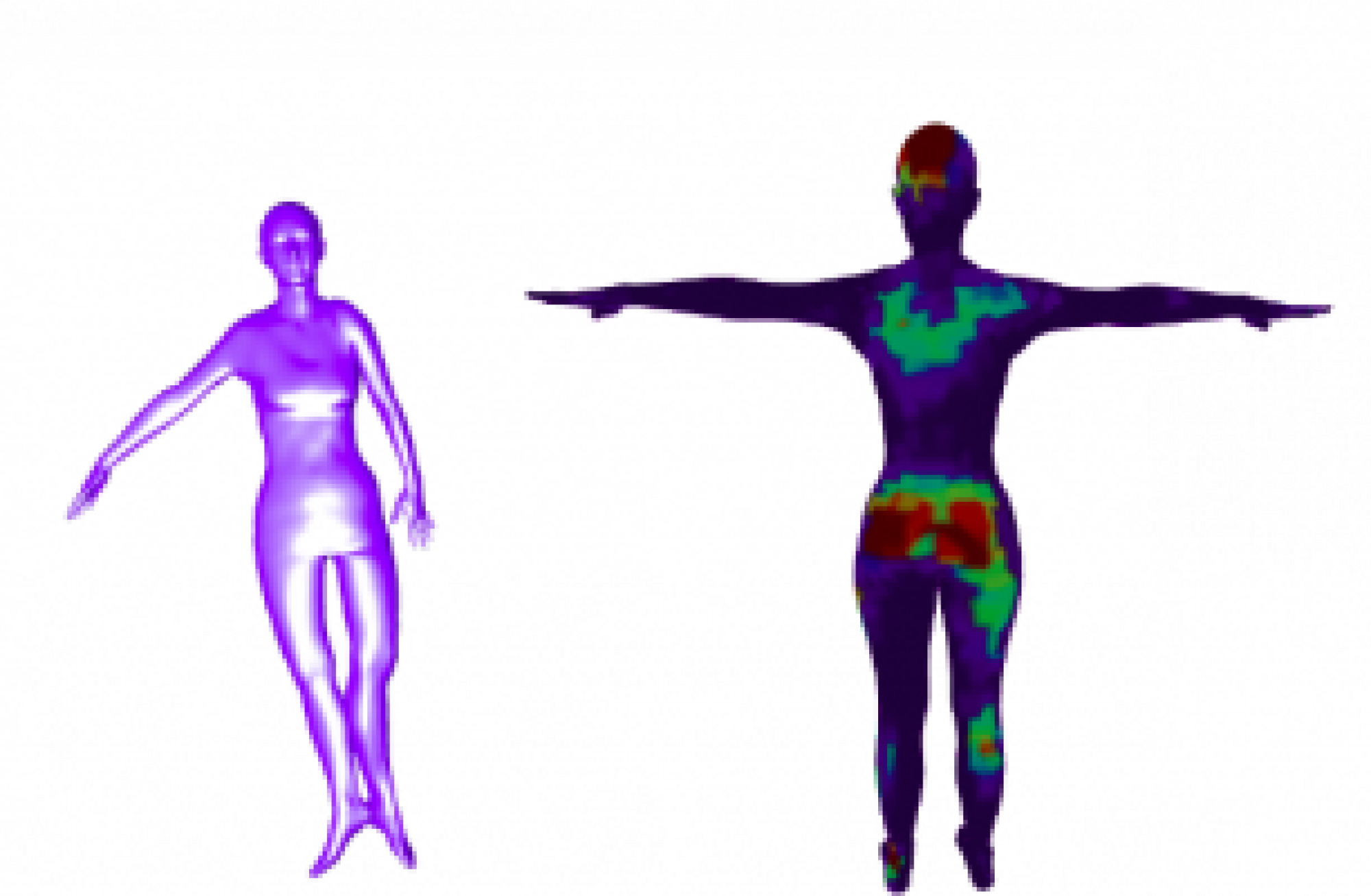
Objective
The objective of the project is to build a system to inform nurses and caregivers where to provide care to prevent pressure ulcers.
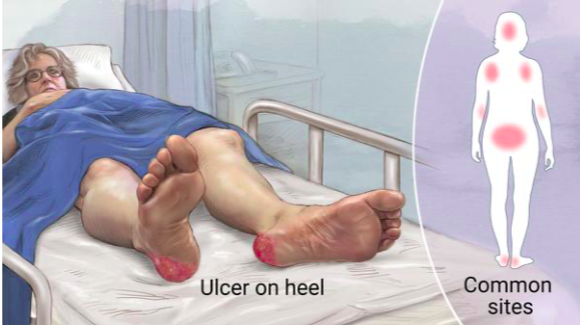
Motivation
Understanding the 3D orientation of people in bed and pressure applied on their bodies, in the form of a 3D pressure map, has immense potential for healthcare applications, especially in preventing pressure ulcers. Current methods focus on singular facets of the problem—predicting only 2D/3D poses, generating 2D pressure images, predicting pressure only for certain body regions instead of the full body, or forming indirect approximations to the 3D pressure map. In contrast, our work concentrates on jointly inferring the human body mesh (3D pose & shape) and 3D applied pressure map across the entire. We introduce BodyMAP, a deep model that directly predicts 3D pressure
on the surface of the human body in bed, jointly with the body mesh. The 3D pressure map is represented as a pressure value at each mesh vertex, enabling precise localization of high pressure regions on the body. Additionally, we present BodyMAP-WS, a new formulation of pressure prediction in which we implicitly learn pressure in 3D by aligning sensed 2D pressure images with differentiable 2D projections of a 3D pressure map. In extensive evaluations with real-world and simulated human data, our method outperforms the current state-of-the-art methods by 24% & 25% on in-bed body mesh and 3D applied pressure map prediction respectively.
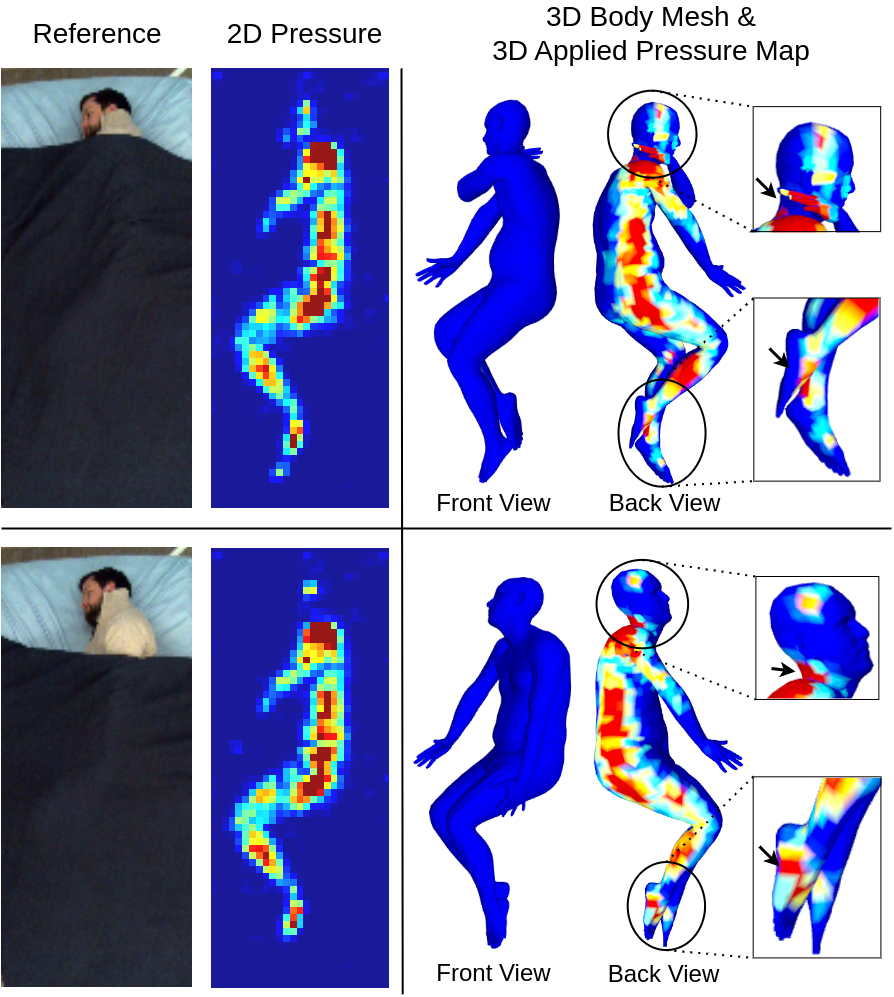
Figure: Distinct 3D poses can have similar 2D pressure images. The insets of the 3D pressure map show pressure being applied to different areas demonstrating its use in localizing pressure that is applied on the human bod
These pressure visualizations show how pressure is distributed over the human body i.e. what are the areas where higher pressure is being applied. Such a pressure mapping system can then be used by caregivers to perform informed repositioning and prevent pressure ulcers.
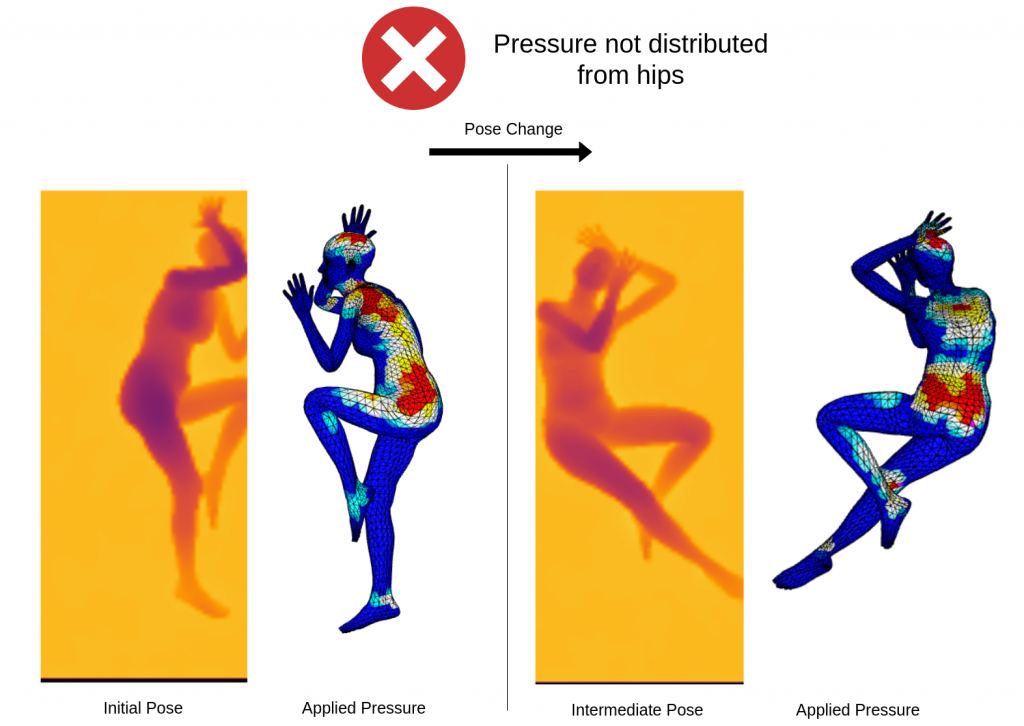
Figure: Pressure Not being distributed after pose change